Features of stigma and their impact on adherence to asthma medication
Stigma about asthma exists and it has been associated with low adherence to medication. However, stigma has commonly been observed as an atomic, irreducible concept, which has most commonly been mentioned in qualitative studies. Stigma has been observed through the lens of a personal tragedy model, whereas stigma about asthma should not only be a problem for asthma patients as it is not rooted only within the scope of their perceptions.
To address this, this study aims to uncover the underlying mechanisms of stigma by taking into account more granular stigma features and assess their individual association with adherence and how coping mechanisms affect each one of these relationships.
A survey about life with asthma was administered online and 545 individual responses were collected in the period between the 1st and the 5th of May in 2020. For the purposes of this analysis, we focused on stigma and stigma-related concepts, adherence behaviors and coping mechanisms. Stigma related factors that were examined were: denial, discrimination, exogenous perceptions (anticipated stigma), the impact of media, disparaging humour and internalized stigma.
Pearson’s Correlations and Linear Regression were used to assess the associations between stigma features and how powerful they are in predicting adherence.
As a second part of the analysis, Mediation analysis (using PROCESS) was conducted to test the mediating effect of coping mechanisms.
Denial was the strongest predictor of adherence to medication, however, other stigma dimensions, exogenous perceptions, and discrimination were also significantly correlated with adherence.
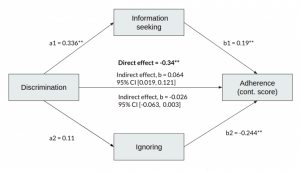
Ignoring asthma, as a maladaptive coping mechanism, was associated with lower levels of adherence. Conversely, information seeking had a positive relationship with adherence.
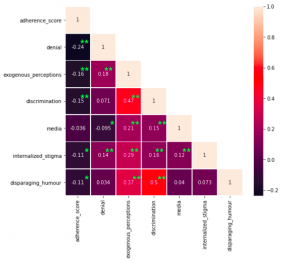
Higher levels of ignoring were associated with higher levels for all stigma features. Interestingly, information seeking did not have such a uniform relationship with features. It was not a valid coping mechanism for exogenous perceptions, it was negatively associated with denial and positively associated with discrimination and disparaging humour.
These results mean that underlying factors of stigmatization have different mechanisms by which they impact patients. In addition, this study highlights that future interventions should focus not only on addressing patient-related stigma factors, but also focus on changing negative public perceptions about asthma.



